The Functions of HLA Genes
The Human Leukocyte Antigen (HLA) system is a group of genes that plays a crucial role in the immune system. Located on the short arm of chromosome 6, the HLA complex is part of the Major Histocompatibility Complex (MHC) in humans, which is responsible for the regulation of the immune system. HLA genes encode cell-surface proteins that are critical for the presentation of foreign antigens to the immune system, enabling it to recognize and respond to pathogens and other harmful substances. This blog post will delve into the diverse functions of the HLA genes and explore their implications in health and disease.
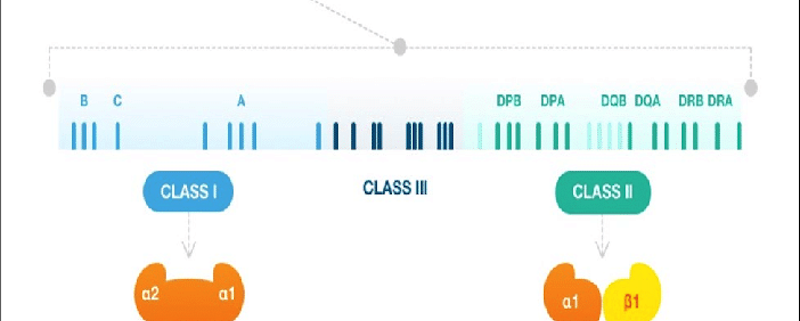
Class I HLA Genes: HLA-A, HLA-B, and HLA-C
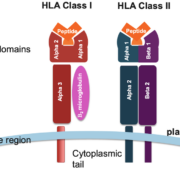
The class I HLA genes include HLA-A, HLA-B, and HLA-C, which code for HLA class I molecules. These molecules are expressed on the surface of almost all nucleated cells and are involved in the presentation of intracellular peptides, such as those derived from viruses or intracellular bacteria, to cytotoxic T lymphocytes (CTLs). When a cell is infected by a pathogen, the HLA class I molecules bind to the pathogen-derived peptides and present them on the cell surface. This alerts the immune system to the presence of the pathogen and triggers a response by the CTLs, which can then destroy the infected cell.
The polymorphic nature of class I HLA genes ensures that individuals have a diverse repertoire of HLA molecules, enabling them to recognize and respond to a wide array of pathogens. This diversity has both positive and negative implications. On one hand, it provides the population with increased resistance to infectious diseases; on the other hand, it increases the risk of autoimmune diseases and complications in organ transplantation due to the possibility of mismatches between donor and recipient HLA molecules.
Class II HLA Genes: HLA-DP, HLA-DQ, and HLA-DR
The class II HLA genes include HLA-DP, HLA-DQ, and HLA-DR, which code for HLA class II molecules. These molecules are primarily expressed on the surface of antigen-presenting cells (APCs), such as macrophages, dendritic cells, and B cells. HLA class II molecules present extracellular antigens, such as those derived from bacteria, fungi, or parasites, to helper T cells (Th cells). This presentation initiates an immune response, which may include the activation of B cells to produce antibodies, macrophages to engulf pathogens, or cytotoxic T cells to directly kill infected cells.
The polymorphism of class II HLA genes contributes to the diversity of the immune response to pathogens, but it also plays a role in the development of autoimmune diseases. Certain HLA class II alleles have been associated with an increased risk of autoimmune diseases such as type 1 diabetes, rheumatoid arthritis, and multiple sclerosis.
HLA Class III Genes: Complement Components and Inflammatory Response
HLA class III genes are not directly involved in antigen presentation, but they play important roles in the immune response. This group includes genes encoding complement components, such as C2, C4, and factor B, which are crucial for the activation of the complement system. The complement system is a group of proteins that, once activated, helps to clear pathogens and damaged cells from the body. The HLA class III region also contains genes involved in the regulation of inflammation, such as tumor necrosis factor (TNF) and lymphotoxin-alpha (LTA).
Implications of HLA Genes in Health and Disease
Given the critical role of HLA genes in the immune system, it’s not surprising that they have been implicated in a variety of health and disease contexts. Some of the most notable implications include:
- Autoimmune diseases: As mentioned earlier, the polymorphism of HLA genes has been associated with an increased risk of autoimmune diseases. In these conditions, the immune system mistakenly attacks the body’s own tissues, leading to inflammation and tissue damage. The specific HLA alleles that confer susceptibility to autoimmune diseases vary depending on the condition. For example, HLA-DRB104 is associated with a higher risk of rheumatoid arthritis, while HLA-DQB10302 is linked to an increased risk of type 1 diabetes.
- Infectious diseases: HLA genes also influence susceptibility to infectious diseases. Certain HLA alleles can provide protection against specific pathogens, while others may increase the risk of infection or severe disease. For instance, the HLA-B57 and HLA-B27 alleles have been found to be protective against HIV progression to AIDS, while HLA-B*35 is associated with rapid disease progression.
- Cancer: The role of HLA genes in cancer is complex and not yet fully understood. Some HLA alleles have been linked to an increased risk of certain cancers, while others may provide protection. For example, HLA-B08 has been associated with an increased risk of Hodgkin’s lymphoma, while HLA-DRB113 is linked to a lower risk of the disease. HLA molecules also play a role in the recognition of tumor antigens by the immune system, which can lead to the elimination of cancer cells or, in some cases, the development of immune tolerance to the tumor.
- Organ transplantation: Matching HLA molecules between organ donors and recipients is crucial for successful transplantation. HLA mismatching can lead to transplant rejection due to the immune system recognizing the transplanted organ as foreign. To minimize the risk of rejection, efforts are made to match the HLA types of donors and recipients as closely as possible. However, the high degree of HLA polymorphism can make finding suitable donors challenging, particularly for patients from ethnic minority populations.
Conclusion
HLA genes play an essential role in the immune system, influencing our ability to respond to and eliminate pathogens, as well as our susceptibility to various diseases. The extensive polymorphism of HLA genes contributes to both the strength and the complexity of the human immune response. As our understanding of the HLA system continues to grow, it holds the potential to inform the development of new therapies and interventions for a wide range of diseases, from autoimmune disorders to cancer.


 The Sequencing Center
The Sequencing Center
Leave a Reply
Want to join the discussion?Feel free to contribute!